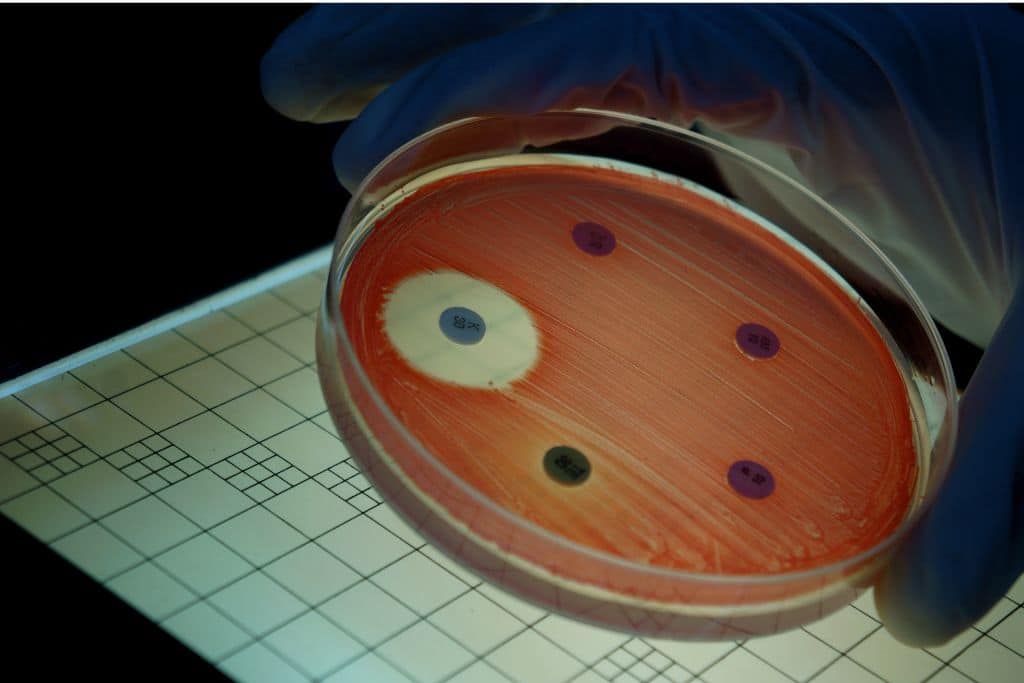
Pollution from farming and pharmaceutical ingredients has increased the risk of antimicrobial resistance in the environment. Pollution from hospitals, effluent from pharmaceutical manufacturing, and the misuse of antimicrobials in managing livestock, have fuelled the rise in superbugs, which experts warn could be responsible for as many deaths as cancer by 2050.
—
In the past two decades, concerns over the growing prevalence of antimicrobial resistance have risen considerably. Along with the lack of sanitation and failure to control sewage in parts of the world, pharmaceutical, and farming pollution is causing a significant rise in superbugs, strains of bacteria viruses, fungi, and parasites that are resistant to antibiotics aimed to kill them.
Antimicrobial resistance is a naturally occurring phenomenon that can be slowed, but not stopped. Since microbial, including bacteria, viruses, and parasites start to adapt to drugs that are intended to kill them, standard treatments in modern medicine may become less effective and even ineffective.
In 2019, antimicrobial resistance was the cause of roughly 5 million deaths. This number is expected to increase greatly in the coming decades if action is not taken to stop the rise of superbugs.
A new United Nations Environment Programme (UNEP) report estimates that by 2050, 10 million people a year could die because of antimicrobial resistance, making it as fatal as cancer. According to the findings, climate change and antimicrobial resistance are two of the prominent threats to global health.
Pharmaceutical ingredients end up in the natural environment, through effluent from the manufacturing process, following patients’ consumption and subsequent excretion, and the improper disposal of unused and expired medicines.
Waterways, untreated sewage, and areas of poor sanitation in the developing world, and a lack of regulation in animal farming have become breeding grounds for resistant bacteria as pharmaceutical pollution continues to increase and threaten global health.
You might also like: What’s the Link Between Climate Change and Disease Outbreaks?
Following their emergence, superbugs can quickly spread and threaten the health of people even in wealthier countries with well-funded healthcare systems.
In the past, superbugs have mostly surfaced in healthcare settings since sick patients or people with weakened immune systems tend to be more susceptible to picking up infections.
However, many antibiotics have been prescribed to people and animals when unnecessary. Hence, the overuse and misuse of antibiotics have been fueling the rise of drug-resistance bacteria. As more people take antibiotics when it is not necessary, superbugs emerge as bacteria become increasingly resistant and they can continue to thrive and spread. Drugs may eventually then become less effective to kill certain types of bacteria.
A University of York-led Global Monitoring of Pharmaceuticals Project discovered that pharmaceutical pollution contamination in water had been found on every continent.
However, the highest levels of cumulative pharmaceutical concentrations are found in sub-Saharan Africa, South Asia, and South America. Contaminated sites are typically areas in low-to-middle-income countries with poor wastewater, waste management infrastructure, and pharmaceutical manufacturing.
While drug resistance can develop organically, the overuse of drugs in livestock and food production has also accelerated the process.
To confront the challenges that surfaced due to antimicrobial resistance, countries have been advised by the World Health Organization (WHO) Action Plan to invest in antimicrobial resistance containment through AMR surveillance. The WHO believes that AMR surveillance is an essential tool to inform policies and infection prevention that could also reduce the reliance on antimicrobials while shifting the focus on technological innovations such as vaccinations and other alternatives to antimicrobials.
The World Economic Forum report published in 2021 stated that animal mortality rates could increase by 1% due to antimicrobial resistance, equating to a loss of US$13 billion in livestock value annually.
The World Bank estimates that by the next decade, the economic impact of antimicrobial resistance could see the gross domestic product worldwide falling $3.4 trillion annually and as a result, push 24 million more people into extreme poverty.
The UN report further pushed for governments and the private sector in the developed world to tackle pollution in the developing world, highlighting that it would be in their self-interest to do so.
The environment continues to play a key role in the development of antimicrobial resistance. More coordinated action with a major focus on prevention at local, national, regional, and global levels is needed to limit the spread of resistant pathogens to preserve modern medicine’s ability to treat diseases in humans and animals.
You might also like: The Environmental Impact of Medical Waste Disposal